Threading the small needle
A veterinarian considers how his profession can make care financially accessible—while maintaining standards and remaining solvent
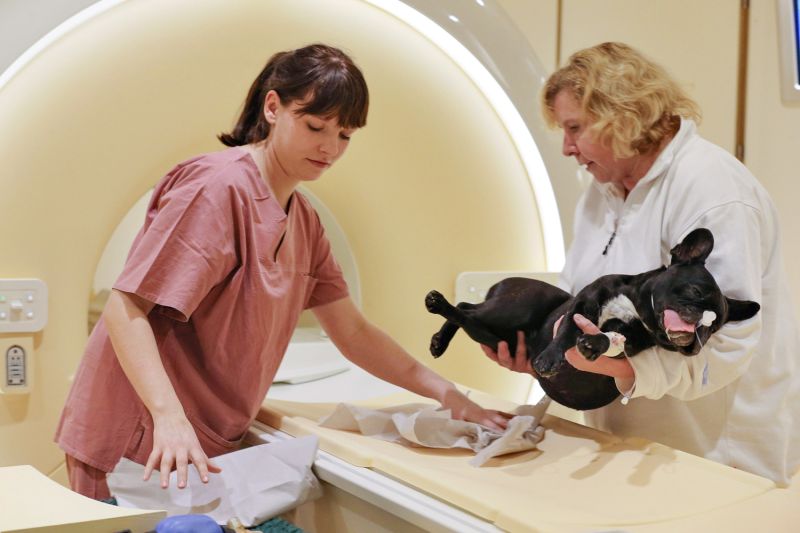
Growing societal recognition of the value pets bring to our lives and continued advances in veterinary medicine would seem to be the perfect recipe for improving animal welfare.
Unfortunately, the same factors that have allowed veterinarians to do remarkable things for the pets of more affluent people—brain surgery, MRIs and cardiac pacemakers, to name a few—have also resulted in a progressively larger percentage of the pet-owning public being effectively “priced out” of quality veterinary care.
In the last 10 years, the cost of veterinary care has outpaced the rate of inflation. Our profession is confronting the fact that without significant changes, pet ownership and its attendant veterinary care may soon become a luxury that only the affluent can afford.
One factor driving the increasing costs of care is the fact that veterinarians, especially those in general practice, are under increasing financial pressure. Annual pet visits are declining, protocols for less frequent vaccinations have decreased revenue, online pharmacies and “big box” pet stores have gutted pharmacy revenues, and many people have gravitated to the internet for veterinary advice.
“Economic euthanasia,” the term used to describe situations where animals with treatable conditions are euthanized because owners simply can’t afford the treatment, is all too common.
Another factor is staggering educational debt currently averaging over $145,000 at graduation. Veterinarians may feel stuck between a rock and a hard place. How do they maintain the financial viability of their businesses while also trying to make veterinary care financially accessible to as many pet owners as possible?
Every veterinarian I have ever known routinely gives away thousands of dollars annually in free or discounted care, but the need greatly outstrips their ability to help every client who can’t afford market rates. “Economic euthanasia,” the term used to describe situations where animals with treatable conditions are euthanized because owners simply can’t afford the treatment, is all too common.
This is not only a tragic outcome for the pet and owner, but a huge source of emotional stress for veterinarians and a prime contributor to compassion fatigue and burnout in the profession. When you consider that, according to a recent study by the U.S. Centers for Disease Control and Prevention, veterinarians have a suicide rate between 2.1 and 3.5 times that of the general population, it becomes clear that access to care is an issue we can’t afford to ignore.
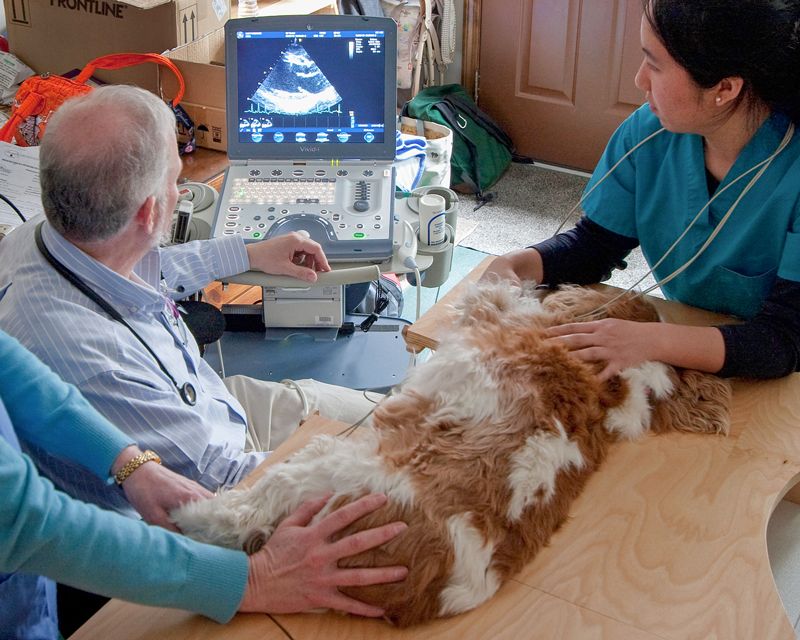
Real-world standards
One potential solution involves a reevaluation of “standard of care,” which refers to the minimum level of acceptable care prescribed in a particular medical situation or, as one court described it, “the care required of and practiced by the average, reasonably prudent, competent veterinarian in the community.” Historically, any care that fell below this standard could be considered malpractice.
The problem is that our profession is sorely lacking in clear and consistent standards. Clinical practice guidelines—commonly used in human medicine to direct ideal care for specific medical conditions— are essentially nonexistent in veterinary medicine. Thus a particular course of treatment in one state could be considered “standard of care,” while the exact same treatment in another state could result in the veterinarian being found guilty of malpractice.
When presented with specific clinical conditions, veterinarians don’t have a centralized reference they can use for guidance on the standard of care. For example: Should vets perform a urine culture on every dog with signs of a urinary tract infection? How many courses of antibiotics should a vet try before culturing the urine? When should a vet recommend bloodwork, an X-ray or ultrasound to check for bladder stones or other causes of infection? Does a 50-percent lower bill justify performing a surgical procedure with a 20-percent lower success rate? Does a 20-percent lower bill justify offering an owner a procedure with a 50-percent lower likelihood of success?
The fact that technology exists doesn’t mean you always have to use it.
These are real-world, financially relevant questions without obvious cookiecutter answers. But there are some basic principles that can help guide vets in a more cost-effective direction.
At the veterinary hospital I co-own, we constantly try to impart to our interns and residents the philosophy of not doing tests if the results won’t change how they (or the pet owner) will treat the patient. We teach them that jumping to running diagnostics without first obtaining a detailed history and performing a thorough physical exam is a recipe for wasting time and the client’s money. And while there is certainly a place for high-tech diagnostics in veterinary medicine, the fact that technology exists doesn’t mean you always have to use it. Sometimes less expensive alternatives are equally effective, and other times the potential benefit of a more expensive intervention may not be justifiable given an only marginally better anticipated outcome or wildly disproportionate cost.
To practice the most intelligent and cost-effective medicine possible, veterinarians must stay up-to-date on the scientific literature, which may suggest new and effective treatment plans. For example, recent studies have found that outpatient therapy for puppies infected with parvovirus was associated with a 75-percent survival rate. While not quite as high as intensive inpatient therapy, this finding highlights the importance of understanding all treatment options and trying to blend them into a coherent plan that fits the client’s budget.
Although standards of care are theoretically designed to set a baseline level of minimally acceptable care, there is increasing recognition that they should instead reflect a continuum of acceptable care that takes into account available evidence- based medicine, client expectations and financial limitations.
Because animals are still considered property in the eyes of the law, and owners are entitled to decide how much to spend on their pet’s care, veterinarians are all too often faced with ill or injured pets whose owners essentially dictate what the standard of care is going to be. Faced with a choice between providing what might be considered substandard care and no care at all, vets will always try to do something to help their patient.
Legally, veterinarians can’t knowingly provide treatment that falls below the standard of care. But the reality is that we are confronted with this issue on a daily basis by our clients’ financial limitations. These legal and financial realities aren’t adequately acknowledged in the commonly accepted veterinary definition of standard of care.
Veterinarians must thread a small needle here. Clients’ financial limitations won’t protect them against malpractice claims, but vets clearly need the flexibility to offer care that fits the client’s budget and is based on the best, up-to-date, evidence-based medicine. It will take a concerted effort to create clinical practice guidelines for veterinary medicine, a national (as opposed to a stateby- state) definition of standard of care, and a uniform approach for state veterinary medical boards assessing cases of potential malpractice. At the same time, veterinarians must thoroughly document medical decisions when treatment is dictated by their clients’ financial constraints.
Although veterinary medicine is decades behind its human counterpart in the use of evidence-based medicine, numerous white papers, consensus statements and specialty organization monographs exist for specific conditions, such as diabetes mellitus and Lyme disease, and for specific treatments, such as the use of anti-inflammatory medications, to name a few.
Unfortunately, these aren’t consistently used by veterinarians for making clinical decisions, nor are they acknowledged by state medical boards, the American Veterinary Medical Association or the American Animal Hospital Association as default standards of care. Creating an accessible clearinghouse of such information would be an excellent first step toward a more consistent and enforceable standard.

The road ahead
Thankfully, there are some indicators that change is coming.
Veterinary educational conferences and professional journals are now delving into access-to-care issues. There has been an uptick in for-profit and nonprofit veterinary clinics that market their services specifically to low-income pet owners, and many states and veterinary professional organizations are creating programs to help subsidize the care of pets in need. Three years ago in my home state, the Rhode Island Veterinary Medical Association and the Rhode Island SPCA joined forces to open the Pets in Need Veterinary Clinic, a full-service clinic that treats the pets of residents with documented financial need.
In another promising development, the Humane Society Veterinary Medical Association helped launch the Access to Veterinary Care Coalition, whose members include vets from private practice, nonprofit clinics and academia, as well as representatives of social service and animal welfare organizations. The group, in conjunction with the University of Tennessee’s College of Social Work, is currently conducting a large-scale study of access-to-care issues to determine the prevalence of the problem, and following data analysis, the coalition will produce a detailed reference that identifies obstacles to obtaining care and makes recommendations for best practices to address this multifactorial problem.
Our veterinary oath instructs us to “protect animal health and welfare and to prevent and relieve animal suffering.”
Failure to ensure access to veterinary care to as many ill, injured and needy animals as possible can only be seen as an abdication of this oath. Veterinarians and the animal protection community must make access to care a defining principle of compassionate and effective veterinary medicine—for the animals whose lives are entrusted to us.








