A crisis for people is a crisis for pets
Flint failure creates uncertainty for animals and their owners
Even after it became public knowledge that some local water samples met the Environmental Protection Agency’s standard for “toxic waste” in 2015, the people of Flint, Mich., were told that bathing was perfectly safe.
It was advice that would cause most people to raise a skeptical eyebrow, and most people haven’t been through what Flint residents have faced: months of official reassurances about their water’s safety that turned out to be false.
After a water-supply switch went awry, the city started using Flint River water as a stopgap measure in April 2014. In October 2014, General Motors stopped using the water because it was corroding car parts; a year later, amid public outcry, the water supply was switched back to its original source, Detroit Water & Sewerage Department.
But much damage had already been done. What residents came to find out wasn’t safe—and hadn’t been for many months—was drinking the water. Or brushing teeth, or boiling food, or washing clothes and dishes. For over a year, some Michigan residents had unknowingly ingested corrosive water that had leached lead from Flint’s water pipes.
The mistake poisoned Michigan’s most vulnerable and poverty-stricken citizens—children started to test positive for lead poisoning. It became clear to Jill Fritz, Michigan senior state director for The HSUS, that pets would also be affected.
“A lot of the city of Flint is very underserved as far as any services, let alone pet care services,” she says. “There are very few veterinary options within the city of Flint, and many people in the city of Flint have no way to get to a veterinarian, so if they get a notice that their animal has tested positive for lead contamination, then what do they do?”
Genesee County Animal Control (GCAC) and the Humane Society of Genesee County in Flint had remained on the Detroit water grid, and thanks to generous donations of bottled water, they were also able to offer safe water to pet owners. But neither had the resources to provide lead testing or care for pets in the community who were already affected.
The Michigan State University (MSU) College of Veterinary Medicine, MSU Extension and the Michigan Department of Agriculture and Rural Development stepped up to create and distribute a factsheet for pet owners and a guide to help veterinarians detect and treat lead poisoning. MSU’s College of Veterinary Medicine also organized and funded lead-testing clinics at churches and other community gathering places, distributed bilingual fliers throughout the city and spread the word via Michigan public radio, a local TV news segment and The Flint Journal.
The community was responsive—two elementary schools asked for clinic fliers to send home with every child, says Kristen Lare Flory, director of the veterinary college’s office of marketing and communications.
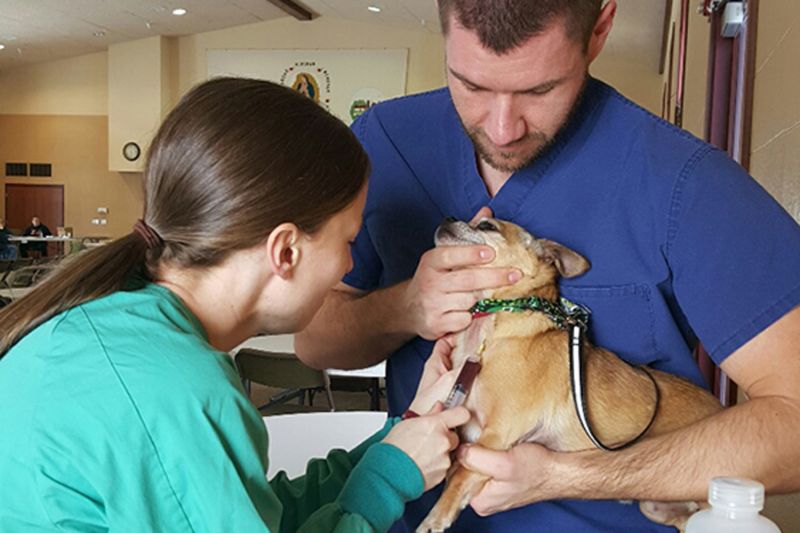
At a GCAC rabies clinic in February, MSU veterinarians offered free lead testing to anyone with a Flint address. Of the almost 70 dogs tested, only a handful had elevated lead levels. But Fritz and others believe that such results may be deceiving: No one knows how many pets were sickened by tainted water over the past year, and without comprehensive testing, it’s impossible to determine how many pets are still affected.
“Those that came in to do [the testing] were really appreciative that we were thinking of the dogs,” says Mike Chaddock, associate dean for administration at the veterinary college. “But I don’t know how many [people] said, ‘I’m not going to do that’ and just walked away.”
“Even if people understand what we’re doing, they’re going to say, ‘I don’t trust anyone who’s part of the government coming out and looking at my dog’ or, ‘I don’t trust Michigan State.’ It’s an entire trust issue,” he says.
Flory also notes that many Flint pet owners likely have no car and may have inflexible work hours, making it difficult for MSU to access and test a representative sample of Flint dogs.
“Getting the word out has been exceedingly difficult,” says Daniel Langlois, assistant professor at MSU’s veterinary college. “We just don’t have the resources or connections.” He notes that many schools were unable to distribute clinic fliers at all because of school regulations, and the news segment covering the clinics had aired at 6 a.m.
On March 5, MSU veterinarians tested another 40 dogs at Our Lady of Guadalupe Church on the edge of the so-called “hot zone,” the affected area on the map that goes “straight down the center line” of Flint, says Flory. And on March 19, just over 60 dogs were tested at St. Paul’s Episcopal Church, directly in the hot zone. GCAC representatives were on hand to offer pet care service vouchers to attendees.
At all three clinics, MSU veterinarians surveyed pet owners, asking questions like “What is the primary water source for your pet?”
“People were almost defensive about it,” says Flory, adding that the overwhelming majority of respondents started giving their dog bottled water as soon as they knew that the tap water was contaminated—“as soon as they knew” being the operative words.
“There’s been a lot of misinformation,” she says, citing widespread “boil water” advisories, even though boiling can actually increase the concentration of lead in the water. Despite such misinformation, Langlois speculates that 80-85 percent of respondents had been giving their pets bottled or filtered water for the past three to four months.
Lead toxicity in dogs can cause vomiting, seizures, blindness and death, and treatment is expensive, time-consuming and sometimes ineffective. With few resources to go toward additional lead-testing clinics, the long-term effects of Flint River water on the city’s animals are still unknown.








